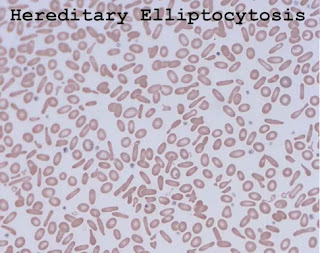
Hereditary elliptocytosis (HE)
- Hereditary Elliptocytosis, or ovalocytosis, is an inherited blood disease in which the RBC is oval rather than the typical biconcave disc formed by the defect of the RBC membrane.
- Hereditary elliptocytosis has an autosomal inheritance pattern.
A subtype of hereditary elliptocytosis, called hereditary granulocytosis (HPP), is inherited in an autosomal recessive manner.
- A clinically significant hemolytic anemia occurs only in 5-10% of sufferers.
Categories:
1. Common hereditary elliptocytosis:
- Asymptomatic carrier status - the individual with no symptoms of the disease and can only diagnosed through blood film.
- Mild disease-asymptomatic patients with mild and compensated hemolytic anemia.
- Sporadic hemolysis - hemolysis occurs in the case of comorbidities (including infection) and vitamin B12 deficiency.
- Neonatal poikilocytosis – poikilocytosis with asymptomatic hemolytic anemia.
- Chronic hemolysis – ranging from moderate to severe symptomatic hemolytic anemia.
- Homozygous or compound heterozygous-from mild hemolytic anemia to life-threatening hemolytic anemia.
- Pyropoikilocytosis (HPP) – common in Africa, a fatal severe hemolytic anemia with micropoikilocytosis.
2. South-east Asian ovalocytosis (SAO) (stomatocytic elliptocytosis):
- Common in South-East Asian countries.
- With mild hemolytic anemia and has increased resistance to malaria infection.
3. Spherocytic elliptocytosis (hereditary hemolytic ovalocytosis)
Accounts for 10% of cases of hereditary elliptocytosis. Compared with typical mild diseases, Elliptocytes cells are less prominent, more spherical, and maybe dominated by spherocytes.
Causes:
- This is due to mutations in certain proteins (pectin, protein 4.1, and glycoprotein C) in the membrane skeleton network responsible for the stability of the red blood cell membrane.
- Defects in any of these proteins will cause a decrease in the mechanical stability of the membrane, leading to fragmentation of the membrane and the production of oval red blood cells.
- Hereditary Pyropoikilocytosis is the severe form of hereditary elliptocytosis, it occurs when the network is too weakened, in these cases, the red blood cells are severely deformed, mimicking the red blood cells destructions caused by exposure to heat.
Clinical Manifestations
- Most cases of HE is asymptomatic, with normal RBC survival and no anemia.
- Numerous are detected when an individual is tested because a child or other relative is found to have elliptocytosis.
- Neonatal hyperbilirubinemia is common and may need an exchange transfusion.
- Some infants with HE suffers from severe hemolytic anemia at birth, with obvious microcytosis and poikilocytosis, similar to hereditary Pyropoikilocytosis.
Such infants usually improve spontaneously, with mild HE at 1 year old.
Diagnosis
- The peripheral blood smear examination is a key diagnostic test.
The presence of more than 15% elliptocytes indicates HE.
- Checking blood smears of parents or siblings may help confirm whether there is a genetic abnormality.
- The cytoskeletal protein can be analyzed, but it is usually not required.
- In most cases of HE, the osmotic fragility test is normal, but in the case of poikilocytosis and elliptocytosis, the osmotic pressure fragility test may be abnormal.
- The mean corpuscular volume in HPP is 50-60 fL with obvious poikilocytosis and red blood cell fragmentation.
- Gene mutation analysis can identify causal mutations to confirm the diagnosis.
Differential diagnosis
You should exclude the other acquired causes of elliptocytic or fragmented red blood cells, such as (ie, iron, vitamin B12, and folic acid deficiency and microangiopathic hemolytic anemia), congenital dyserythropoietic anemia, and alpha and beta-thalassemia.
Treatment
- Most of the Hereditary elliptocytosis patients do not need any treatment.
- Splenectomy is not curative, but it may be beneficial in the few severe cases that require treatment.
Prognosis
- Hereditary elliptocytosis has a good prognosis, and only patients with very serious diseases can shorten their lifespan.



Comments
Post a Comment