Case study (36) – Anemia of Renal Failure
The blood film comes from a 35-year-old man whose blood count is as follows:
Hemoglobin (Hb) 63 g/L
Mean corpuscular volume (MCV) 81 fL
White blood cells (WBC) 6.1 X 109/L
Platelets 137 X 109/L
Questions:
Q1. What is the diagnosis?
Q2. What is the pathogenesis of the anemia?
Q3. What other hematological complications may occur?
Answers:
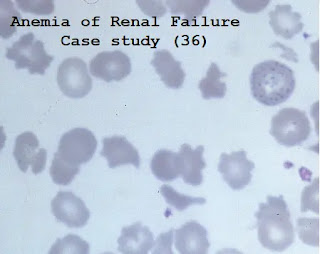
A1. This patient is suffering from renal failure. The blood film shows characteristic echinocytes (Burr cells).
The reticulocyte count is commonly normal or slightly reduced, and bone marrow examination appears normoblastic erythropoiesis, frequently without the erythroid hyperplasia expected for the level of anemia.
A2. The most important pathogenic mechanism is reduced production of erythropoietin by diseased kidneys.
The treatment has been revolutionized by the availability of recombinant erythropoietin (EPO).
Red blood cell survival rate is reduced, iron deficiency caused by blood loss (for example, during hemodialysis) and secondary hyperparathyroidism are contributing factors.
Most patients with renal failure will receive EPO treatment.
An important result of EPO administration is the development of functional iron deficiency (FID) – characterized by the presence of serum ferritin and bone marrow iron reservoirs to assess that iron is not fully incorporated into developing erythroblasts in normal iron reservoirs.
Many modern analyzers allow rapid assessment of the percentage of hypochromic cells (%HRC); the assessment of reticulocyte hemoglobin content (CHr) is also informative.
The soluble transferrin receptor assay (sTfR) and serum transferrin concentration can also provide useful information.
The importance of diagnosing FID is that intravenous iron supplementation should be considered as soon as possible.
A3. Other hematological complications of renal failure include
- Polycythemia, for example, following ectopic EPO production by renal tumors or cysts.
- Defects in platelet function, leading to a hemorrhagic diathesis partly correctable by 1-deamino-8-d-arginine vasopressin (DDAVP)
- Hypercoagulability, especially in nephrotic syndrome, is related to reduced partial fibrinolysis, reduced protein C, and reduced antithrombin.
- Changes caused by underlying pathological changes that cause kidney failure (eg autoimmune hemolytic anemia of systemic lupus erythematosus and idiopathic thrombocytopenic purpura; low platelet count in diffuse intravascular coagulation)
- Treatment-induced changes (e.g. immunosuppression)
The Blood film below shows Burr cells and basophilic stippling in another patient with renal failure.



Comments
Post a Comment