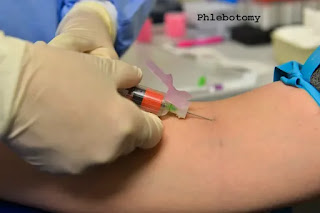
Phlebotomy - is the process of making an incision in a vein with a needle.
- Phlebotomy is the process of making an incision in a vein with a needle.• The procedure is known as a venipuncture.
• A person who performs phlebotomy is called a phlebotomist, although doctors, nurses & medical laboratory scientists.
Duties of a Phlebotomist
- The correct ID of the client before collection.- Collection of the appropriate amount of blood for the specified tests.
- Selection of the appropriate specimen container.
- Correct labeling of all specimens with the required information.
- Appropriate transportation back to the lab on time.
- Effective interaction with clients and hospital personnel.
- Performance of related computer operations and record keeping.
- Observation of all safety rules.
- Attendance at continuing education.
Venipuncture:
• Venipuncture is the process of obtaining blood samples from veins for laboratory testing, it is probably the most common procedure in the medical field, usually performed for the following reasons:1. To obtain blood samples to perform diagnostics.
2. To collect blood for later use should the patient’s condition requires transfusions.
3. To remove blood that was found with excessive levels of erythrocytes or iron.
The equipment necessary to perform a Venipuncture
Devices Used for Drawing Blood:
• Lancet – The lancet was first used before 5th century B.C. the practitioner manually perforated the vein. Many shallow cuts were sometimes made.• Spring-Loaded Lancet – Came into use during the early 18th century. The device was cocked, and a “trigger” fired the spring-driven blade into the vein.
• The Fleam – Used during the 18th century. Many varieties existed. Sometimes a wooden “fleam stick” was used to strike the back of the blade and drive it into the vein.
• Scarificator – The scarificator, a series of twelve blades, was also in trend during the 18th century. The device was cocked, and the trigger released spring-driven rotary blades that caused many shallow cuts. The scarificator appears more humane than other bloodletting instruments. Blood was caught in shallow bowls.
• Flint Cup – throughout the 17th to 19th centuries, blood was also cached in small flint cups. The heated air inside the cup generated a vacuum causing blood to flow into the cup, a handy technique for drawing blood from a localized area. This practice was called ‘cupping’.
• Leeches – (Hirudo medicinalis); Leeches were “enticed” by “leeches” to attach themselves to the skin. The area was chosen, and a drop of milk or blood was the bait. Once the leech was engorged, it could drop off. In the early 1800s, the little animal became quite scarce, and leech farms were having difficulty keeping up with the demand. Therefore, they became quite expensive.
Avoid performing venipuncture on:
1. The arm on side of mastectomy. If drawn here, the test results could be inaccurate because of lymphedema.2. Scarred or burned areas. Performing a venipuncture at these sites is more difficult due to the scar tissue.
3. Arm in which blood is being transfusion / IV cannula. The fluid in the IV might dilute the specimen.
4. A hematoma (A hematoma is an abnormal collection of blood outside of a blood vessel. It occurs because the wall of a blood vessel wall, artery, vein, or capillary, has been damaged and blood has leaked into tissues) If drawn here, could cause incorrect test results.
5. Edematous (Edema is swelling caused by fluid retention) should be avoided because the accumulated fluid could alter test results.
Blood can be collected from 3 different sources:
I. Venous blood.
Most are required because most majority of routine tests are performed on venous blood. Blood can be taken directly from the vein.
- The best site for venous collection is the deep veins of the ante-cubital fossa.
- If difficult to obtain from the ante-cubital fossa we can draw blood from the following various site:
1. Femoral vein:
2. Dorsum of hand vein:
3. Jugular vein.
4. Scalp vein.
These sites -other than the forearm- require extra caution and expertise for the collection of blood.
• Tourniquet.
• Vacutainer or syringe.
• Alcohol swab.
• Bandage/ mediplast.
2. Explain the procedure and purpose of the patient.
3. Assess the patient's physical disposition (i.e. diet, exercise).
4. Position the patient - sitting or lying (NEVER allow the patient to sit upright on a high stool or standing due to the possibility of syncope).
5. Check the requisition form for requested tests, patient information, and any special requirements.
6. Select a suitable site for venipuncture.
7. Prepare the equipment, the patient, and the puncture site.
8. An appropriate syringe and/or needle should be selected.
9. If multiple specimens are to be collected it’s better to use a butterfly needle.
- Attach the needle to the holder
- Place the tube into the holder
10. The tourniquet should be applied to the upper arm.
11. Sterilize the puncture area with a spirit/alcohol swab and allow it to dry.
12. Visualize and palpate the vein.
13. Do not enter the vein directly and vertically.
Because there is more chance of puncturing the other side of the venous wall in this way.
- Hold vein in place
- Insert needle
14. Draw blood according to required tests.
15. Withdraw the needle. Loosen the tourniquet.
16. Press down on the gauze, applying adequate pressure.
17. Apply a piece of band or mediplast.
18. Dispose of contaminated material in the designated container.
19. Put blood into a suitable container.
20. While the tube fills, remove the tourniquet.
21. Label the collection tubes in the drawing area.
22. Immediately send the specimens with the requisition to the laboratory.
Tourniquets should not be applied for a long time and not more than 1 min. To avoid stasis of blood.
Stasis increases the concentration of RBC hemoglobin albumin calcium.
Blind attempts to puncture the vein should not be made.
Subcutaneous manipulation of the needle to enter a vein
should not be done as it causes a lot of pain.
Once the needle is withdrawn, pressure should be applied and maintained for 1-2 minutes.
If you cannot control the pressure this will cause Ecchymoses i.e. extravasation of blood.
- Collect quickly, fill, and seal both ends immediately.
- No air bubbles.
- Put in ice water and deliver STAT to the lab
2. Temporal artery
3. Femoral Artery
- For infants and young children.
Blood can be obtained from:
1. Heel pulp
- Automatic lancet device
2. Finger bulb
3. Ear lobule
How to collect capillary blood?
- Select the least used finger.
- Cleanse the site with an alcohol swab.
- Puncture across the grain of the skin, then transfer blood to a strip or small container.
Blood Specimen Collection and Processing:
•The first step in acquiring a quality lab. The test result for any patient is the specimen collection procedure.
• Blood specimens are obtained through capillary skin punctures (finger, toe, heel), arterial, or venous sampling.
• Capillary / dermal /skin puncture, earlobe stick, finger stick, heel stick (infants).
• Venous puncture (direct puncture of the vein by venipuncture).
•Automatic sample mixing reduces repeat collections due to clots and hemolysis.
•Collect even the smallest drops from the puncture site with no squeezing, scooping or stopping to mix the sample blood immediately.
• Probing is not recommended. Probing is painful for the patient. In most cases another puncture in a site below the first site, or use of another vein on the other arm, is advisable.
• It is advisable not to attempt a venipuncture more than twice. Notify the patient’s Registered Nurse
• Another person should attempt to draw the specimen
• If another person is asked to draw a patient, the new person must re-identify the patient.
- If an incomplete collection or no blood is obtained Change the position of the needle. Move it forward (it may not be in the lumen)
• or move it backward (it may have penetrated too far).
• Adjust the angle (the bevel may be against the vein wall).
• Re-anchor the vein. Veins sometimes go away from the point of the needle and puncture site.
- If blood stops flowing into the syringe/tube
• The vein may have collapsed; resecure the tourniquet to increase venous filling. If this fails, remove the needle, take care of the puncture site, and redraw.
• The needle may have pulled out of the vein when switching tubes. Hold equipment gently and place fingers against the patient's arm, using the flange for leverage when withdrawing and inserting tubes.
• Wear gloves and a lab coat or gown when handling blood/body fluids.
• Change gloves after each patient or when contaminated.
• Wash hands frequently.
• Dispose of items in appropriate containers.
• Dispose of needles immediately upon removal from the patient's vein. Do not bend, break, recap, or resheath needles to prevent accidental needle puncture or splashing of contents.
• Clean up any blood spills with a disinfectant such as freshly made 10% bleach.
• If you stick yourself with a contaminated needle:
• Remove your gloves and dispose of them properly.
• Squeeze puncture site to promote bleeding.
• Wash the area well with soap and water.
• Record the patient's name and ID number.
• Follow the institution's guidelines regarding treatment and follow-up.
To prevent a hematoma
• Puncture only the uppermost wall of the vein (just under the skin)
• Remove the tourniquet before removing the needle
• Use the major superficial veins (the large veins just under the skin)
• Make sure the needle fully penetrates the uppermost wall of the vein. (partial the puncture may allow blood to leak into the tissues just under the skin)
• Apply pressure to puncture site
Petechiae consist of extravasated blood. This complication could be a result of a coagulation abnormality, such as a platelet defect, and should be brought to the attention of the patient’s healthcare provider.
An automatic nervous system reaction, (psychosomatic trigger), usually based on fear.
Treatment and safe handling of an unconscious patient is a necessity of any qualified Phlebotomist.
• Abort draw: Remove tourniquet, needle, and bend the arm
• Call for assistance.
• Using good body mechanics, slide patient to floor, keeping a hand firmly behind the cervical spine area. Protect the head and neck from injury!
• Elevate feet above the heart and monitor blood pressure, breathing, etc.
• Use ammonia only if the patient is not responsive within 5 minutes and blood pressure remains low.
• Assist to an upright position in stages (monitor B/P with each change in position)
this is a gradual process. If the patient stands up to quickly, he will be most likely to faint again due to a drop in B/P.
- The best site for venous collection is the deep veins of the ante-cubital fossa.
- If difficult to obtain from the ante-cubital fossa we can draw blood from the following various site:
1. Femoral vein:
2. Dorsum of hand vein:
3. Jugular vein.
4. Scalp vein.
These sites -other than the forearm- require extra caution and expertise for the collection of blood.
Blood collection Tools:
Material:• Tourniquet.
• Vacutainer or syringe.
• Alcohol swab.
• Bandage/ mediplast.
Phlebotomy procedure Steps:
1. Wash hands. Apply gloves.2. Explain the procedure and purpose of the patient.
3. Assess the patient's physical disposition (i.e. diet, exercise).
4. Position the patient - sitting or lying (NEVER allow the patient to sit upright on a high stool or standing due to the possibility of syncope).
5. Check the requisition form for requested tests, patient information, and any special requirements.
6. Select a suitable site for venipuncture.
7. Prepare the equipment, the patient, and the puncture site.
8. An appropriate syringe and/or needle should be selected.
9. If multiple specimens are to be collected it’s better to use a butterfly needle.
- Attach the needle to the holder
- Place the tube into the holder
10. The tourniquet should be applied to the upper arm.
11. Sterilize the puncture area with a spirit/alcohol swab and allow it to dry.
12. Visualize and palpate the vein.
13. Do not enter the vein directly and vertically.
Because there is more chance of puncturing the other side of the venous wall in this way.
- Hold vein in place
- Insert needle
14. Draw blood according to required tests.
15. Withdraw the needle. Loosen the tourniquet.
16. Press down on the gauze, applying adequate pressure.
17. Apply a piece of band or mediplast.
19. Put blood into a suitable container.
20. While the tube fills, remove the tourniquet.
21. Label the collection tubes in the drawing area.
22. Immediately send the specimens with the requisition to the laboratory.
Precaution:
The venipuncture area must be cleaned/sterilized properly.Tourniquets should not be applied for a long time and not more than 1 min. To avoid stasis of blood.
Stasis increases the concentration of RBC hemoglobin albumin calcium.
Blind attempts to puncture the vein should not be made.
Subcutaneous manipulation of the needle to enter a vein
should not be done as it causes a lot of pain.
Once the needle is withdrawn, pressure should be applied and maintained for 1-2 minutes.
If you cannot control the pressure this will cause Ecchymoses i.e. extravasation of blood.
II. Arterial blood.
Especially required for estimation of blood gases (ABG): PH, CO2, and O2.- Collect quickly, fill, and seal both ends immediately.
- No air bubbles.
- Put in ice water and deliver STAT to the lab
Arterial blood can be obtained from a superficial artery such as:
1. Radial and brachial artery2. Temporal artery
3. Femoral Artery
III. Capillary blood.
- To draw only a small amount of blood in a microtube or strip for blood sugar and bleeding time tests.- For infants and young children.
Blood can be obtained from:
1. Heel pulp
- Automatic lancet device
2. Finger bulb
3. Ear lobule
How to collect capillary blood?
- Select the least used finger.
- Cleanse the site with an alcohol swab.
- Puncture across the grain of the skin, then transfer blood to a strip or small container.
Blood Specimen Collection and Processing:
•The first step in acquiring a quality lab. The test result for any patient is the specimen collection procedure.
• Blood specimens are obtained through capillary skin punctures (finger, toe, heel), arterial, or venous sampling.
• Capillary / dermal /skin puncture, earlobe stick, finger stick, heel stick (infants).
• Venous puncture (direct puncture of the vein by venipuncture).
New vein finder devices:
• Devices that utilize laser/infrared technology for Vein Viewer (vein finders). E.g. (Veinlite, AccuVein, VeinViewer Flex)New Device for Infant Blood Collection:
- Such as Innovac Quick-Draw•Automatic sample mixing reduces repeat collections due to clots and hemolysis.
•Collect even the smallest drops from the puncture site with no squeezing, scooping or stopping to mix the sample blood immediately.
Problems obtaining a specimen:
- Blood Sample That Cannot Be Obtained:• Probing is not recommended. Probing is painful for the patient. In most cases another puncture in a site below the first site, or use of another vein on the other arm, is advisable.
• It is advisable not to attempt a venipuncture more than twice. Notify the patient’s Registered Nurse
• Another person should attempt to draw the specimen
• If another person is asked to draw a patient, the new person must re-identify the patient.
- If an incomplete collection or no blood is obtained Change the position of the needle. Move it forward (it may not be in the lumen)
• or move it backward (it may have penetrated too far).
• Adjust the angle (the bevel may be against the vein wall).
• Re-anchor the vein. Veins sometimes go away from the point of the needle and puncture site.
- If blood stops flowing into the syringe/tube
• The vein may have collapsed; resecure the tourniquet to increase venous filling. If this fails, remove the needle, take care of the puncture site, and redraw.
• The needle may have pulled out of the vein when switching tubes. Hold equipment gently and place fingers against the patient's arm, using the flange for leverage when withdrawing and inserting tubes.
Safety and infection control
Due to contacts with sick patients and their specimens, it is important to follow safety and infection control procedures.Protect yourself:
• Practice universal precautions:• Wear gloves and a lab coat or gown when handling blood/body fluids.
• Change gloves after each patient or when contaminated.
• Wash hands frequently.
• Dispose of items in appropriate containers.
• Dispose of needles immediately upon removal from the patient's vein. Do not bend, break, recap, or resheath needles to prevent accidental needle puncture or splashing of contents.
• Clean up any blood spills with a disinfectant such as freshly made 10% bleach.
• If you stick yourself with a contaminated needle:
• Remove your gloves and dispose of them properly.
• Squeeze puncture site to promote bleeding.
• Wash the area well with soap and water.
• Record the patient's name and ID number.
• Follow the institution's guidelines regarding treatment and follow-up.
Patient complications
Problems other than an incomplete collection- Hematoma
A hematoma forms under the skin near to the puncture site - release the tourniquet immediately and withdraw the needle. Apply firm pressure.To prevent a hematoma
• Puncture only the uppermost wall of the vein (just under the skin)
• Remove the tourniquet before removing the needle
• Use the major superficial veins (the large veins just under the skin)
• Make sure the needle fully penetrates the uppermost wall of the vein. (partial the puncture may allow blood to leak into the tissues just under the skin)
• Apply pressure to puncture site
Petechiae
Little red spots, ranging in size from pinpoint to several millimeters in diameter.Petechiae consist of extravasated blood. This complication could be a result of a coagulation abnormality, such as a platelet defect, and should be brought to the attention of the patient’s healthcare provider.
Syncope (fainting)
Patients may become dizzy and faint at the thought or sight blood, this is the most common complication phlebotomy. It is caused because of a rapid fall in blood pressure.An automatic nervous system reaction, (psychosomatic trigger), usually based on fear.
Treatment and safe handling of an unconscious patient is a necessity of any qualified Phlebotomist.
• Abort draw: Remove tourniquet, needle, and bend the arm
• Call for assistance.
• Using good body mechanics, slide patient to floor, keeping a hand firmly behind the cervical spine area. Protect the head and neck from injury!
• Elevate feet above the heart and monitor blood pressure, breathing, etc.
• Use ammonia only if the patient is not responsive within 5 minutes and blood pressure remains low.
• Assist to an upright position in stages (monitor B/P with each change in position)
this is a gradual process. If the patient stands up to quickly, he will be most likely to faint again due to a drop in B/P.








Comments
Post a Comment